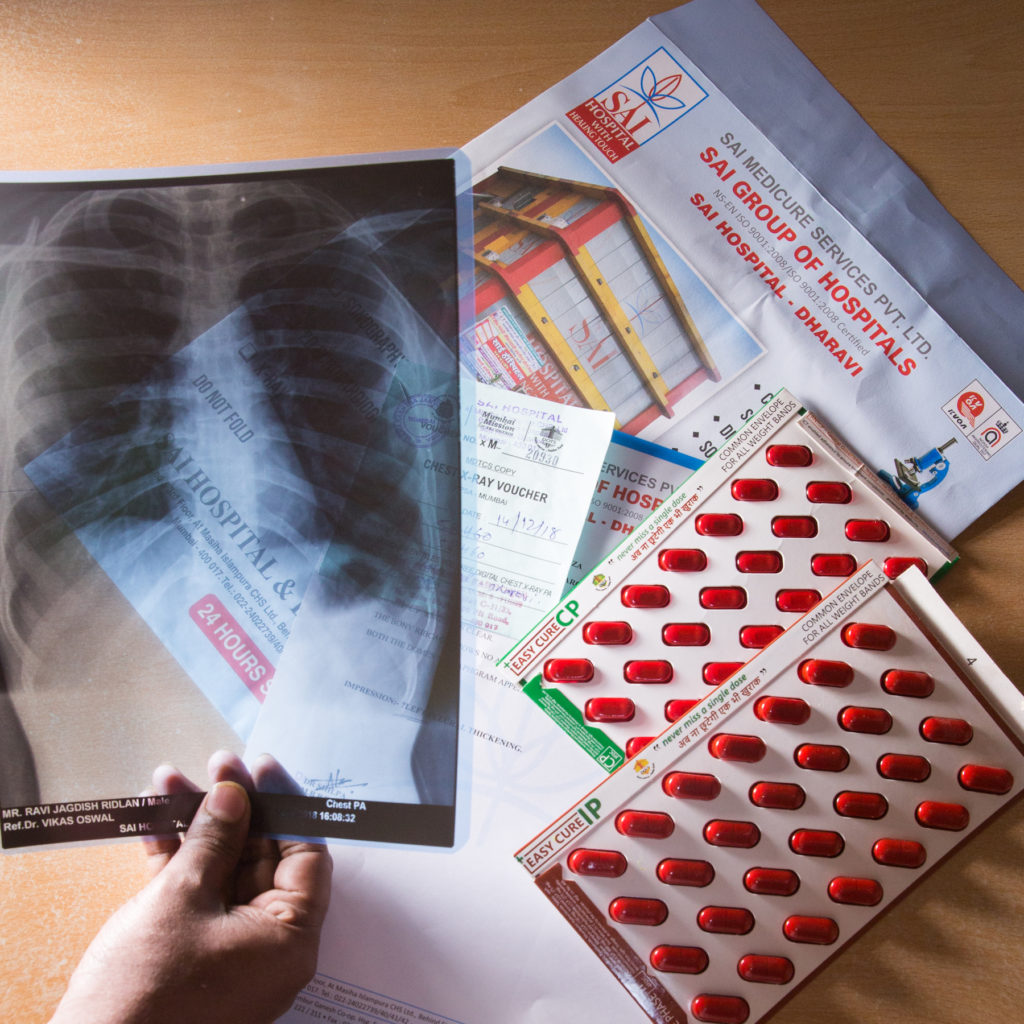
Tuberculosis (TB)
TB is the leading cause of death from a single infectious agent, surpassing HIV/AIDS and one of the top ten causes of death worldwide. According to the Global Tuberculosis report of 2018, 10 million people are estimated to have developed TB globally in 2017. India continues to be the largest contributor to the global TB burden. The challenge is exacerbated due to high rates of drug resistance to conventionally used anti-TB drugs which leads to an increasing occurrence of the more severe form of TB, drug resistant TB (DR-TB). India currently has the highest burden of DR-TB in the world.
The Indian government aims to eliminate TB by 2025. In order to eliminate TB, we must first know how many cases exist across the country. There is under notification of TB cases in India with an estimated 1 million missing TB cases. One key reason for the lack of case notifications stems from the fact that more than 70% of the country’s TB patients seek care in the private sector, where TB cases are not adequately notified in government information systems.
To tackle this challenge, PATH helped develop a private sector engagement model called PPIA which connected patients in the private sector with free TB drugs in the public sector for increased case notifications and treatment outcomes. The model mapped private providers, pharmacists and diagnostic laboratories in Mumbai, who worked together to help create some astounding results: over 60,000 case notifications, 50,000 TB patients initiated on treatment, 28,000 treatments completed, all in approximately 2 years.
The success of the PPIA model led to the Global Fund supported JEET (Joint Effort to Eliminate Tuberculosis) project which Centre for Health Research and Innovation is a part of along with Clinton Foundation and FIND. This pan-India scale up of the private-public linkage model in collaboration with the Government of India, is in line with the government’s National Strategic Plan to eliminate TB by 2025.
The JEET project, through the linkages it creates between the public and private sector, will have a multi-pronged impact in the form of early diagnosis, greater notifications in the private sector and better treatment success. The pan India scale up of the private sector engagement model is expected to touch 3.5 million lives in 22 states across 400 cities.
Maternal Newborn Child Health & Nutrition (MNCHN)
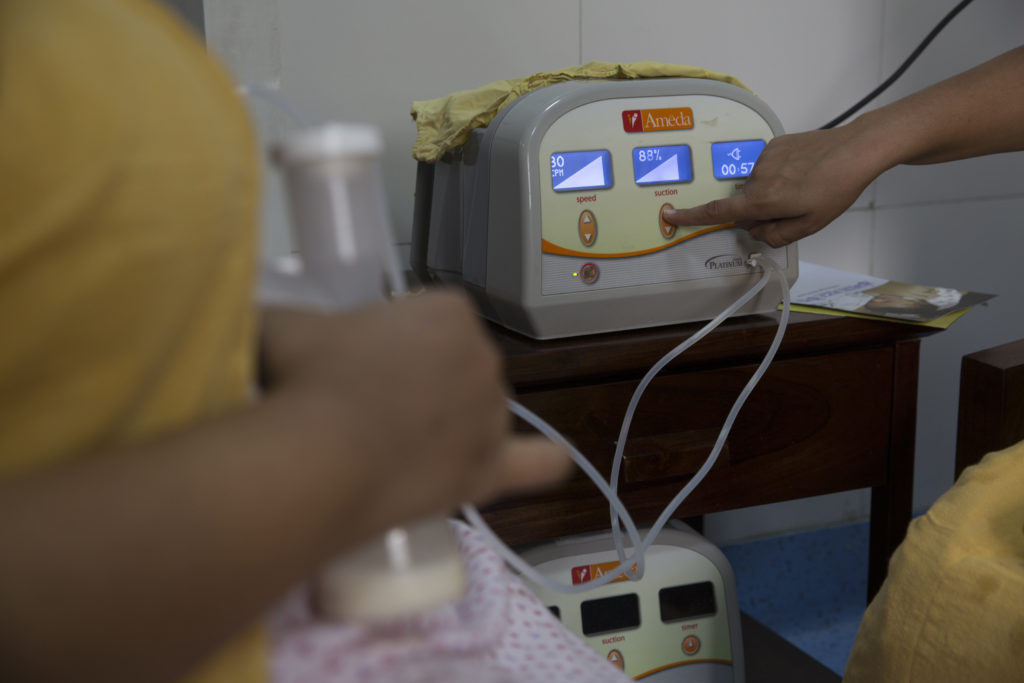
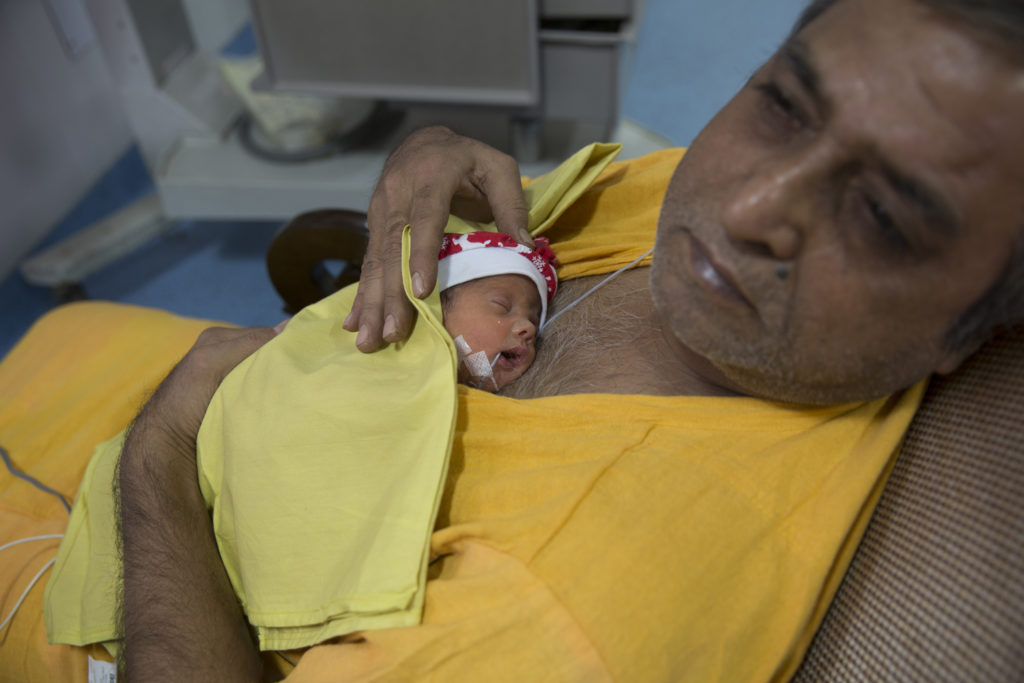
In collaboration with Philips, Centre for Health Research and Innovation is helping to setup or upgrade several Comprehensive Lactation management Centres (CLMCs) across India. There are 60 CLMCs across India currently. CLMCs are integrated lactation centres that provide breastfeeding and breast milk donation support to mothers and also safely collect, process, store and dispense donor human milk to sick and vulnerable babies.
Prematurity is the leading cause of neonatal mortality (NMR) and morbidity in India and globally. In India, each year, 3.5 million babies are born preterm; the highest in the world. Nearly, 71% of all prematurity-related deaths can be averted using cost-effective interventions, of which, breastfeeding is the most powerful. Estimates suggest that early and exclusive breastfeeding can prevent approximately 160,000 under-five deaths in India. Yet, breastfeeding rates remain low.
Although India currently has 57 human milk banks, these are not enough to meet the growing demand for donor human milk (DHM). Centre for Health Research and Innovation is working with PATH to provide technical support to the government in scaling up CLMCs, Lactation Management Units (LMUs), and Lactation Support Units (LSUs) across the country to improve access to human milk.
Dengue, Chikungunya and Malaria
Dengue is the most extensively spread mosquito-borne disease; endemic in more than 100 countries. In India, dengue cases have been reported from all the states, putting the entire population at risk. Overall, between 2015- 2019, 6,55,094 cases have been reported with 1094 deaths.
Chikungunya, which shares the vector with dengue, re-appeared following 32 years of absence of viral activity in 2005. In 2019, 9477 confirmed cases were reported in India.
CHRI with technical assistance from PATH is supporting the National Vector Borne Disease Control Program of the Government of India in dengue and chikungunya prevention and control, along with malaria elimination related activities.
The project aims to reduce the burden of dengue, chikungunya, and malaria cases in the intervention cities. This can be achieved by reducing case fatality rate, enabling faster response to disease outbreaks, making an Integrated Vector Management Plan that can be translated in other geographies and involvement of private practitioners in reporting suspected dengue, chikungunya, and malaria cases.
Contact Us
If you would like to partner us to accelerate healthy equity, please email us.